Whenever you save a new or pending Ortho contract that contains at least one insurance charge schedule, you are prompted to create a pre-authorization claim.
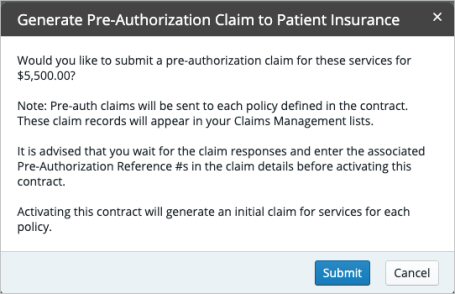
To create the pre-authorization claim, click Submit. A pre-authorization claim is generated for each defined insurance schedule, and the pending contract is saved.

The code(s) entered in the contract's CDT for Initial Billing and Addl. CDT for Initial Claim fields are submitted on the claim.
Note: If you click Cancel from this prompt, you are prompted to activate the claim. It is recommended that you wait for the payer response before activating the contract. See the following section for more information.
Activating the Contract: Now vs. Later
If you click Cancel from the Generate Pre-Authorization Claim prompt, you receive the following prompt:
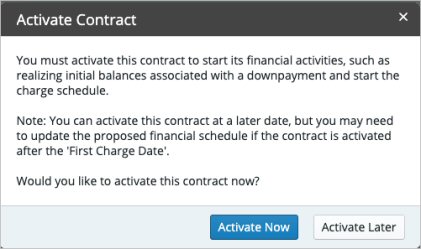
- Select Activate Now to activate the contract. The initial service claim(s) are generated, and the initial contract charges are posted to the ledger.
- Select Activate Later to save the contract in a pending state. You can generate pre-authorization claims at a later time by clicking the Send Pre-Authorization hyperlink in the Contract Summary section of the pending contract.
Providing Additional Information
Pre-authorization claims generated from ortho contracts default to a Needs Info or Pending Review status, depending on your configuration.
To provide the required information:
- Click the View Claim link in the notification message, or select Patient > Insurance > Claims Management and select the claim. The Claim Summary is displayed.
- Click the Edit Addl Info button at the bottom of the summary. The Additional Claim Information window is displayed.
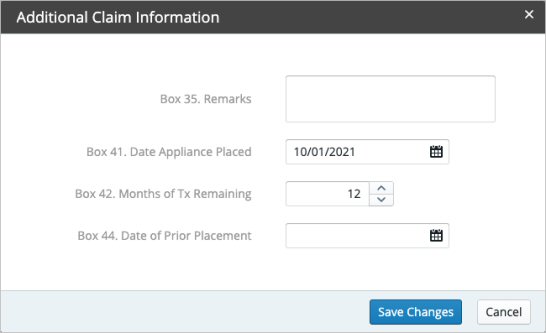
- Enter the relevant information and click Save Changes.
- From the Claim Summary, click Submit Claim.
Once the payer response is received, access the claim from the Claims Management screen, add the reference number to the Claim Summary, and then activate the contract. The pre-authorization claim(s) details are included with the initial service claim(s).
Comments
0 comments
Please sign in to leave a comment.